US Quiz of the Month – Fevereiro 2024
Case Report
We present a case of a 34-year-old female patient with a history of atopic dermatitis who was referred to our center with a 6-month history of nausea, vomiting, early satiety, diffuse abdominal pain and diarrhea (4-5 Bristol 7 stools per day without blood or mucus).
Laboratory analysis revealed anemia (Hemoglobin 11.6 g/dL), eosinophilia (14800×10^3/uL) and C-reactive protein of 6.9 mg/L (N <3.0). Food allergy panel, celiac serology (tissue transglutaminase IgA), anti-nuclear antibody, and anti-neutrophil cytoplasmic antibodies were performed and were negative. Stool calprotectin was 125ug/g (N <30), and stool microscopy for ova and parasites and serologies for Strongyloides and Toxocara species were negative. No abnormal findings were observed in upper endoscopy (including biopsies of corpus, antrum, and duodenum) and colonoscopy (including biopsies of left and right colon).
Magnetic resonance enterography revealed, in right lower abdominal quadrant, discontinuous segments of ileal wall thickening (8mm) with 5 cm of extension each with abnormal contrast enhancement.
Retrograde single-balloon enteroscopy, with progression 120 cm proximally to ileocecal valve, showed edema and atrophic mucosa of ileum up to the limit of progression – mucosal biopsies were taken with identification of 30 intraepithelial eosinophils/ high-power field.
Bowel ultrasound revealed extensive (5cm) segment of ileal wall thickening (9.6mm) located in right lower abdominal quadrant, at the expense of hypertrophy of the muscular layer, maintaining preserved the normal stratification of small bowel wall layers (fig 1.) with increased vascularization of the wall (Limberg score 2) (fig 2). It was associated with mesenteric fat hypertrophy (fig 1.) and a small amount of abdominal free fluid, predominately in the right iliac fossa (fig 3.). There was no evidence of adenopathies or loop dilations.
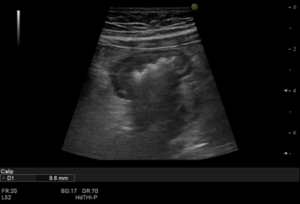
Figure 1.– Illustration of ileal involvement (bowel wall thickening, >3mm) and mesenteric fat hypertrophy by ultrasound.
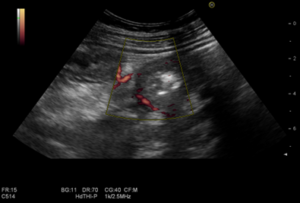
Figure 2.– Illustration of indirect signs of small bowel inflammation by ultrasound – Power doppler small bowel enhancement (Limberg 2).
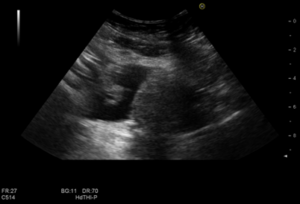
Figure 3.– Illustration of abdominal free fluid by ultrasound.
What is the most likely diagnosis?
Discussion
As the most likely diagnosis was eosinophilic gastroenteritis, and other relevant differential diagnosis were excluded, an initial attempt with a six-food elimination diet was tried without success. Systemic corticosteroids (prednisolone) were initiated with favorable clinical, laboratorial and imagiologic response. After 8 weeks of treatment, small bowel ultrasound was repeated, and no significant findings were observed. Nevertheless, the patient had 2 relapses following the initial response, and azathioprine was introduced with cessation of systemic corticosteroids. No further relapses occurred since then.
Eosinophilic gastroenteritis (EGE) is a rare and benign inflammatory disorder that predominantly affects the stomach and the small bowel, being more frequent in female adults between the 3rd and 5th decade of life. Higher socioeconomic status, Caucasian race and excess weight may be risk factors. Concomitant allergic disorders, including asthma, rhinitis, eczema and drug or food intolerances, are reported in half of the patients.
An accurate diagnosis of EGE poses a significant challenge to clinicians, with evidence of the following three criteria required: Suspicious clinical symptoms, histologic evidence of eosinophilic infiltration in the bowel and exclusion of other pathologies with similar findings.
EGE can be divided into three subtypes (mucosal, muscular and serosal) according to Klein’s classification, and its manifestations depend on the involved intestinal segments and layers.
The natural history and disease course of EGE are not well defined but most patients have chronic disease that will require long-term maintenance treatment.
The management of EGE is based on limited evidence and varies based upon the severity of symptoms and the presence of malabsorption/malnutrition. Systemic corticosteroids, remain the mainstay of treatment. However, given its frequently chronic natural history, maintenance therapy is usually necessary with other options with better safety profiles, including budesonide, dietary restrictions and steroid-sparing agents, such as leukotriene inhibitors, azathioprine, anti-histamines and mast-cell stabilizers.
References
(1)Abou Rached A, El Hajj W. Eosinophilic gastroenteritis: Approach to diagnosis and management. World J Gastrointest Pharmacol Ther. 2016;7(4):513-23.
(2) Limberg B, Osswald B. Diagnosis and differential diagnosis of ulcerative colitis and Crohn’s disease by hydrocolonic sonography. Am J Gastroenterol. 1994;89(7):1051-7.
Authors
Tiago Lima Capela123, Vítor Macedo Silva123, Tiago Cúrdia Gonçalves123, Sílvia Leite123, José Cotter123
- Gastroenterology Department, Hospital Senhora da Oliveira, Guimarães, Portugal.
- Life and Health Sciences Research Institute (ICVS), School of Medicine, University of Minho, Braga/Guimarães, Braga, Portugal.
- ICVS/3B’s, PT Government Associate Laboratory, Guimarães/Braga, Braga, Portugal.2.


